Leg Swelling FAQs.
Answers to your most common questions about Leg Oedema, Lymphoedema, and Lipoedema.

Frequently Asked Questions
Leg Oedema
Leg oedema is swelling caused by a build-up of fluid in the tissues of the legs, ankles, or feet. It can affect one or both legs and may be temporary or long-term.
Common causes include venous disease (poor vein function), heart, kidney, or liver conditions, prolonged sitting or standing, pregnancy, certain medications, and recent surgery or injury.
Swelling is more concerning if it is sudden, painful, affects only one leg, or is associated with chest pain, shortness of breath, redness, or fever.
Pitting oedema means that when you press on the swollen area, a dent remains for a few seconds. This suggests fluid build-up rather than fatty tissue.
Your clinician may examine your legs and arrange blood tests, an ultrasound scan, heart or kidney tests, and review your medications to find the cause.
Treatment depends on the cause and may include leg elevation, regular movement, compression stockings, reducing salt intake, and medications such as diuretics in selected cases.
Yes. Properly fitted compression stockings improve circulation and help reduce fluid build-up and discomfort.
Yes. Gentle walking and ankle or calf exercises help move fluid back toward the heart and reduce swelling.
Staying active, avoiding long periods of sitting or standing, maintaining a healthy weight, and following medical advice can reduce the risk.
If swelling is persistent, worsening, painful, or associated with breathlessness, chest pain, skin redness, or fever.
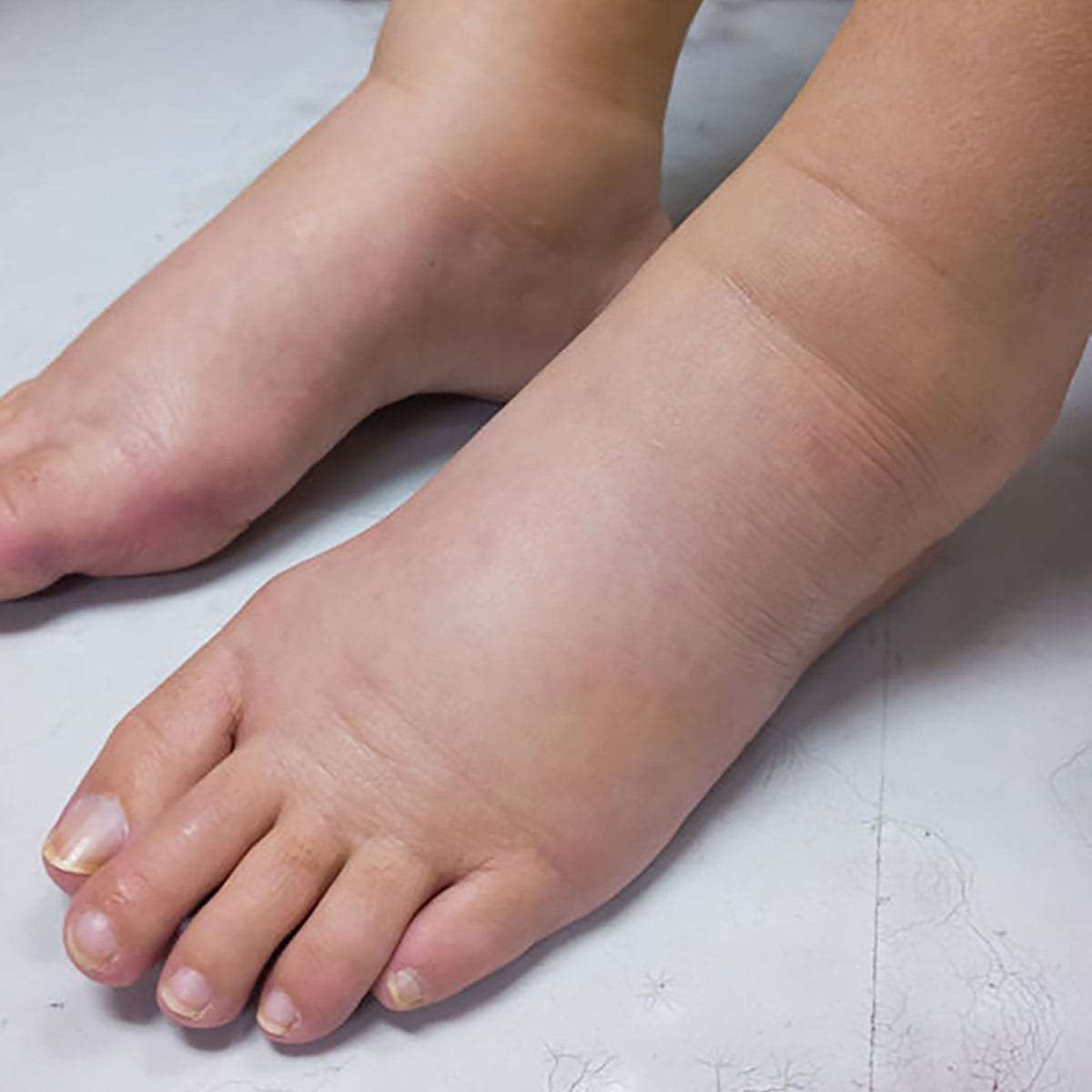
Lymphoedema
Lymphoedema is long-term swelling caused by a problem with the lymphatic system, which normally drains excess fluid from body tissues.
It can be primary (due to inherited lymphatic problems) or secondary, often caused by surgery, radiotherapy, infection, cancer, or injury to lymph vessels or lymph nodes.
There is no cure, but it can usually be well controlled with proper treatment and ongoing self-care.
Early signs include a feeling of heaviness, tightness, or mild swelling that may come and go, often worse at the end of the day.
Diagnosis is based on clinical assessment, limb measurements, and sometimes imaging tests such as ultrasound or lymphatic scans.
Treatment includes compression therapy, manual lymphatic drainage, skin care, exercise, and specialist physiotherapy programs.
Swollen skin is more prone to infection. Keeping the skin clean and moisturised helps prevent cracks and infections such as cellulitis.
Yes. Gentle, regular exercise improves lymph flow and helps maintain strength and movement. Activities should be guided by a healthcare professional.
Cellulitis is a bacterial skin infection. Lymphoedema increases the risk because fluid build-up makes it easier for bacteria to enter the skin.
If the limb becomes suddenly red, hot, painful, or you develop fever or flu-like symptoms.
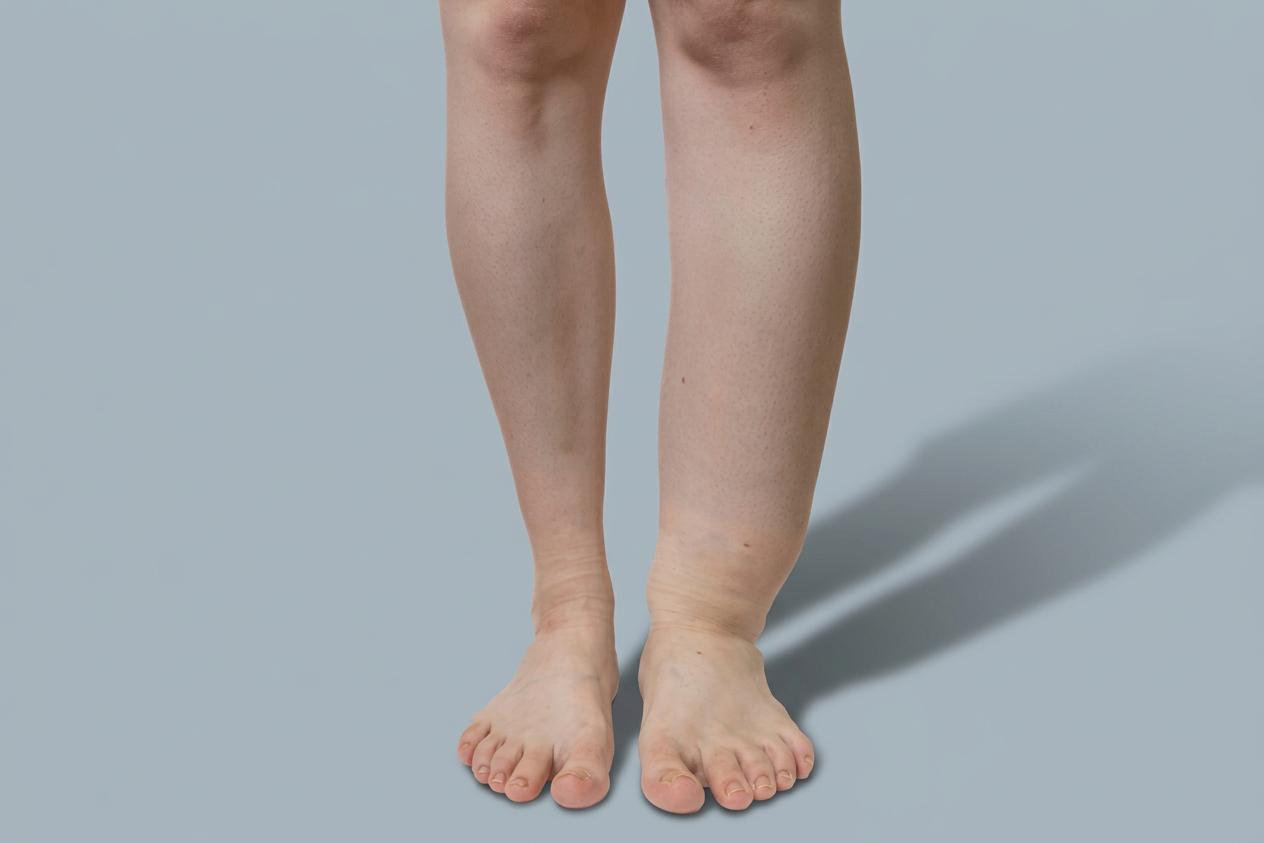
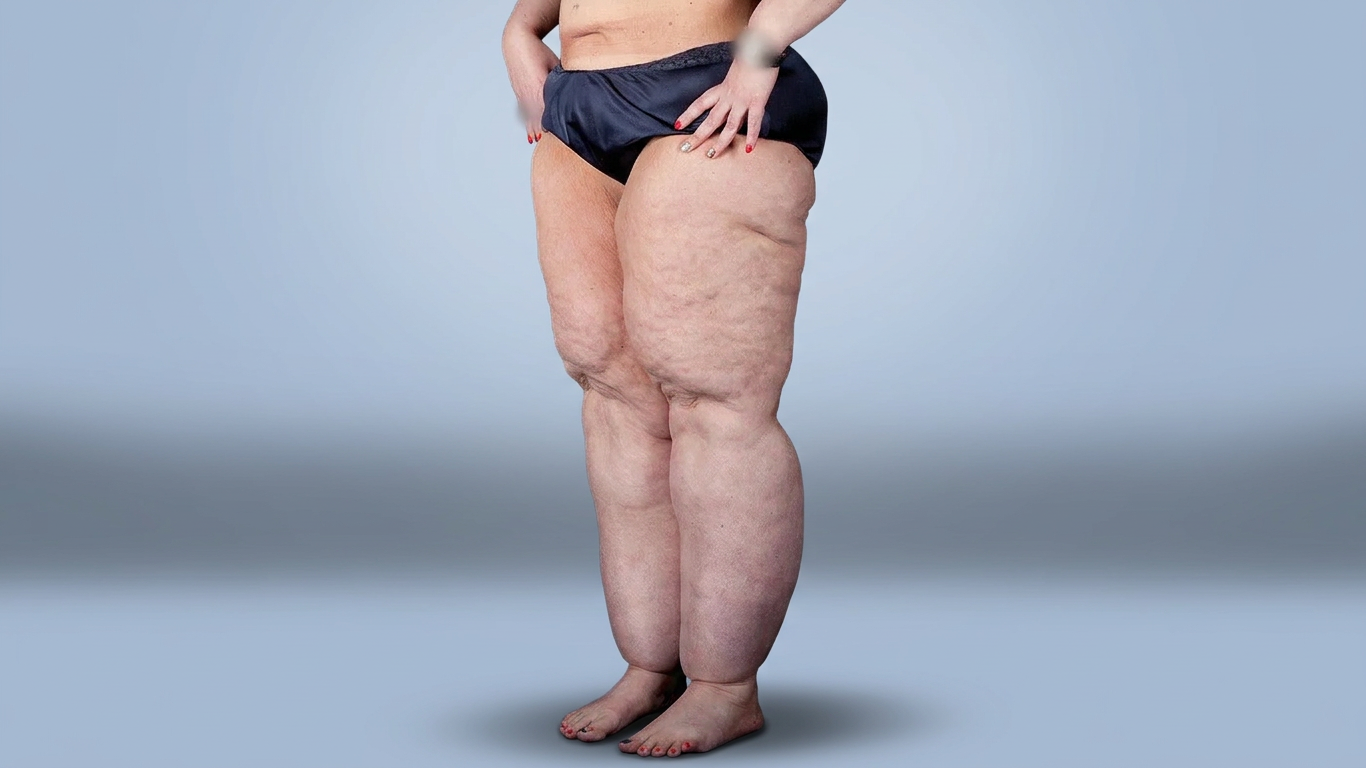
Lipoedema
Lipoedema is a long-term condition involving an abnormal build-up of painful fatty tissue, usually in the legs and sometimes the arms. It most commonly affects women.
Lipoedema fat is resistant to diet and exercise and is often painful, tender, and associated with easy bruising, unlike general body fat.
The exact cause is unknown, but it is believed to be linked to hormones and genetics. It often develops or worsens during puberty, pregnancy, or menopause.
Symptoms include symmetrical enlargement of the legs, tenderness or pain, easy bruising, a feeling of heaviness, and usually little or no swelling in the feet.
Diagnosis is based on medical history and physical examination. Imaging tests may be used to rule out other causes of swelling.
Yes. In advanced stages, fluid build-up can occur on top of the fatty tissue. This is known as lipo-lymphoedema.
Treatment focuses on symptom control and includes compression garments, gentle exercise, manual lymphatic drainage, and overall weight management for general health.
In selected cases, specialist liposuction techniques may be considered and should be discussed with a specialist experienced in treating lipoedema.
Low-impact activities such as walking, swimming, cycling, and water-based exercise are usually best tolerated.
Support is available through specialist clinics, physiotherapists, lymphoedema services, and patient support groups.
Ready to restore your vascular health?
Share your goals with the Pulse Health team and receive a treatment plan tailored to your circulation and lifestyle.
Phone: 0800 45 45 99
Email: info@pulsehealth.nz
Office Address: 1/39 Ghuznee Street, Te Aro 6011, Wellington
