Leg Ulcers FAQs.
Answers to your most common questions about leg ulcers, their causes, and treatments.

Frequently Asked Questions
Understanding Leg Ulcers
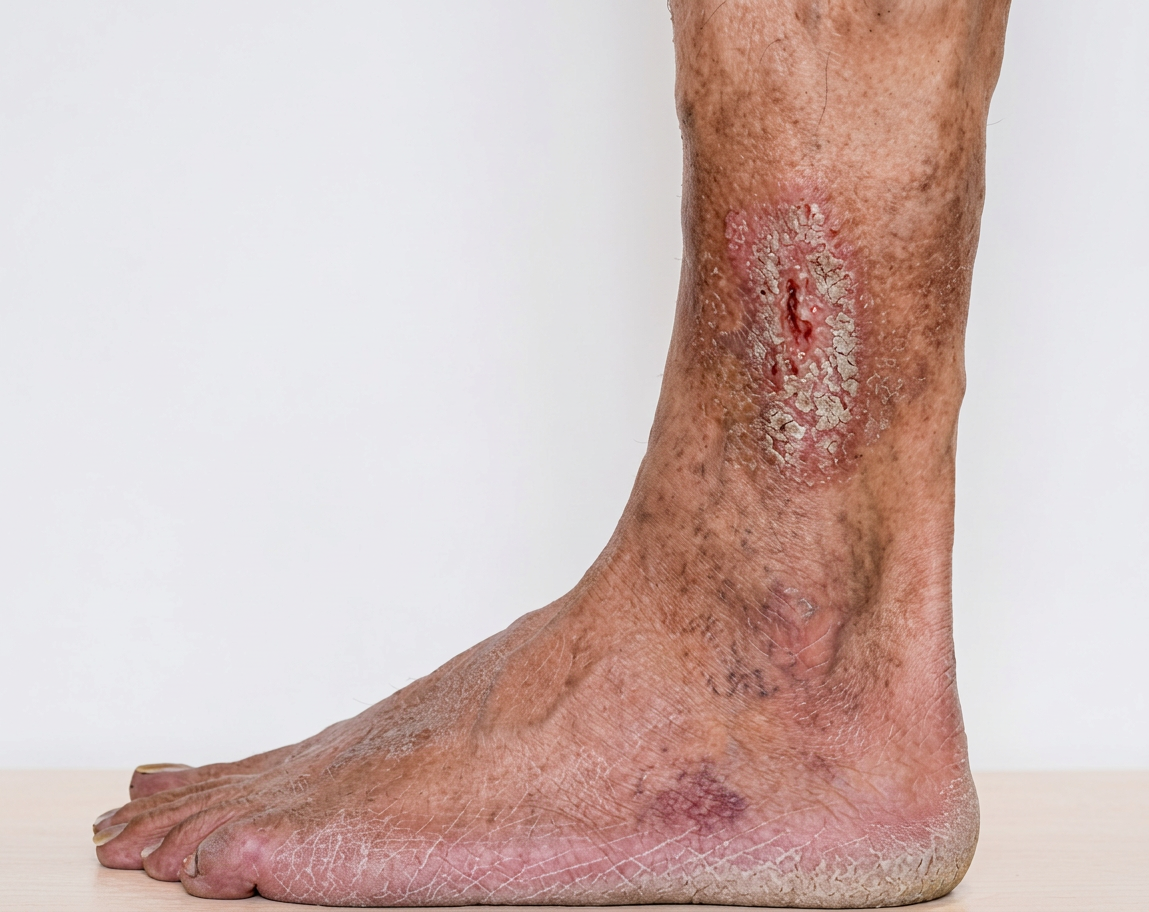
A leg ulcer is an open sore on the skin of the lower leg or ankle that does not heal within a few weeks. They can be painful and may leak fluid or become infected if not treated properly.
Most leg ulcers are caused by poor blood circulation. The main types are:
- Venous ulcers – caused by weak veins or damaged valves that allow blood to pool in the legs (the most common type)
- Arterial ulcers – caused by reduced blood flow due to narrowed or blocked arteries
- Diabetic (neuropathic) ulcers – caused by nerve damage and poor circulation in people with diabetes
- Mixed ulcers – a combination of venous and arterial disease
- Traumatic ulcers – caused by an injury that does not heal properly
- Skin cancers – caused by more advanced skin cancers which result in overlying skin loss with ulceration
Symptoms may include:
- An open wound that is slow to heal
- Swelling, aching, or heaviness in the leg
- Skin changes, such as darkening or hardening around the ankle
- Fluid leakage or crusting
- Pain, especially when standing or walking
- Signs of infection, such as redness, warmth, or discharge
You may be at higher risk if you have:
- Varicose veins or chronic venous disease
- Diabetes
- Poor circulation or peripheral arterial disease
- A history of blood clots (DVT)
- Obesity
- Limited mobility
- Previous leg injuries or surgery
Your clinician will examine the ulcer and your legs and may arrange:
- Ultrasound scans to check blood flow in your veins and arteries
- Blood pressure tests at the ankle (ABPI) to assess circulation
- Blood tests or swabs if infection is suspected
- A biopsy to test tissue if there is concern about skin cancer
Treatment & Healing
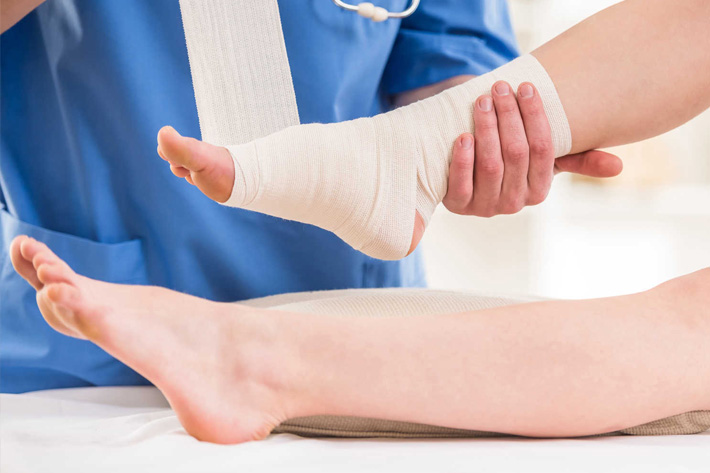
Treatment usually focuses on improving blood flow and helping the wound heal. This may include:
- Compression therapy (bandages or medical compression stockings)
- Regular wound dressings and cleaning
- Elevating the leg to reduce swelling
- Treating underlying vein problems, such as with endovenous ablation or sclerotherapy
- Excision if a skin cancer is identified
Arterial ulcers require treatment to improve blood supply, which may include:
- Medications to improve circulation
- Lifestyle changes, such as stopping smoking
- Referral to a vascular specialist for angioplasty or surgery
- Excision if a skin cancer is present
Healing time varies depending on the cause and your overall health. With proper treatment:
- Some ulcers may heal within weeks to a few months
- Long-standing or complex ulcers may take longer and require specialist care
Yes. Leg ulcers can recur, especially if the underlying circulation problem is not managed. Wearing compression stockings, staying active, and following your treatment plan can significantly reduce the risk.
Prevention & Next Steps
You can reduce your risk by:
- Wearing compression stockings if recommended
- Keeping active and avoiding long periods of sitting or standing
- Elevating your legs when resting
- Maintaining a healthy weight
- Managing conditions such as diabetes and high blood pressure
- Looking after your skin and treating minor injuries promptly
You should seek medical advice if:
- A wound does not heal within two weeks
- The ulcer becomes more painful, red, or swollen
- You notice signs of infection, such as discharge or fever
- You have diabetes or poor circulation and develop any open sore
Yes. Treating underlying vein problems can improve healing and reduce the chance of ulcers returning. Your clinician can advise whether vein treatment is suitable for you.


Ready to restore your vascular health?
Share your goals with the Pulse Health team and receive a treatment plan tailored to your circulation and lifestyle.
Phone: 0800 45 45 99
Email: info@pulsehealth.nz
Office Address: 1/39 Ghuznee Street, Te Aro 6011, Wellington
