Types of Leg Ulcers.
Understanding the different types of leg ulcers is the first step towards effective treatment and restoring skin health.

Varicose Leg Ulcers
What is a Varicose Ulcer?
A varicose ulcer (venous ulcer) is a form of venous ulcer caused by long-standing varicose veins and chronic venous disease. Enlarged and twisted veins allow blood to flow backward and pool in the lower leg, increasing pressure and damaging the skin over time.
These ulcers usually appear around the inside of the ankle and are often associated with visible bulging veins, leg heaviness, aching, swelling, and skin changes such as redness, dryness, or dark staining before the ulcer forms.
For example, a person who stands for long hours at work may develop worsening varicose veins and later notice itchy, discoloured skin near the ankle that eventually breaks down into an open sore.
Book an Assessment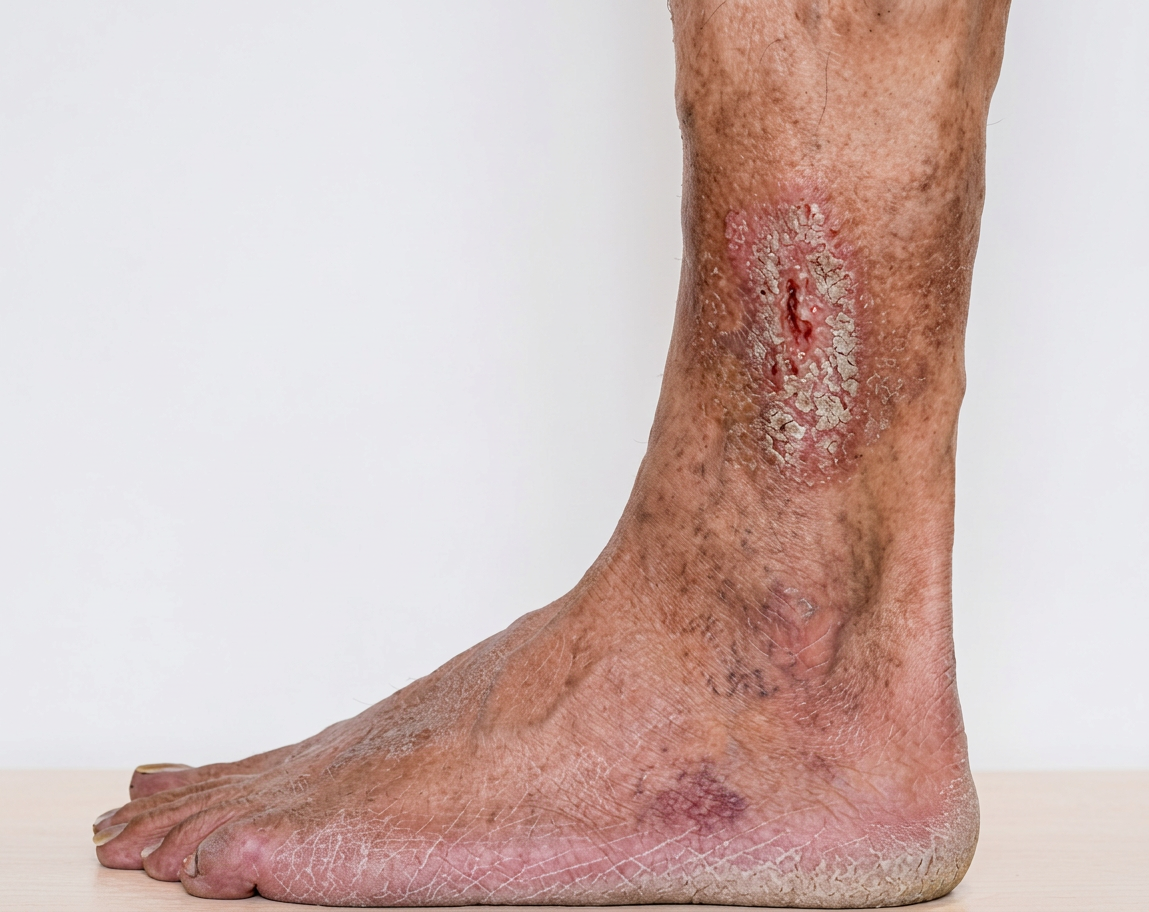
How We Treat Varicose Ulcers
Diagnosis involves a clinical examination and a venous ultrasound scan to map the veins and assess valve function. Leakage of the valves leads to a condition called venous insufficiency, which is the underlying cause of varicose veins.
Treatment includes wound care, compression therapy, and treatment of the underlying varicose veins. Varicose vein treatment with endovenous ablation (Venaseal, RFA) or sclerotherapy can close the leaking veins and reduce the chance of the ulcer returning.
Ongoing care usually includes wearing compression stockings and maintaining an active lifestyle.
Explore Vein Treatments
Arterial Leg Ulcers
What is an Arterial Ulcer?
An arterial leg ulcer is an open sore caused by reduced arterial blood flow to the leg due to narrowed or blocked arteries. This means the skin and tissues do not receive enough oxygen and nutrients to stay healthy and repair themselves.
Arterial ulcers often develop on the toes, heel, foot, or the outer part of the ankle. They tend to be deeper than venous ulcers and are often very painful, especially at night or when the leg is raised. The surrounding skin may look pale, bluish, or shiny and may feel cool to the touch. Hair growth on the leg or foot may be reduced.
Examples include people with a long-term smoking history or diabetes who develop a painful sore on a toe that does not heal, or someone with known peripheral arterial disease who notices increasing pain and a wound on the foot.
Schedule a Consultation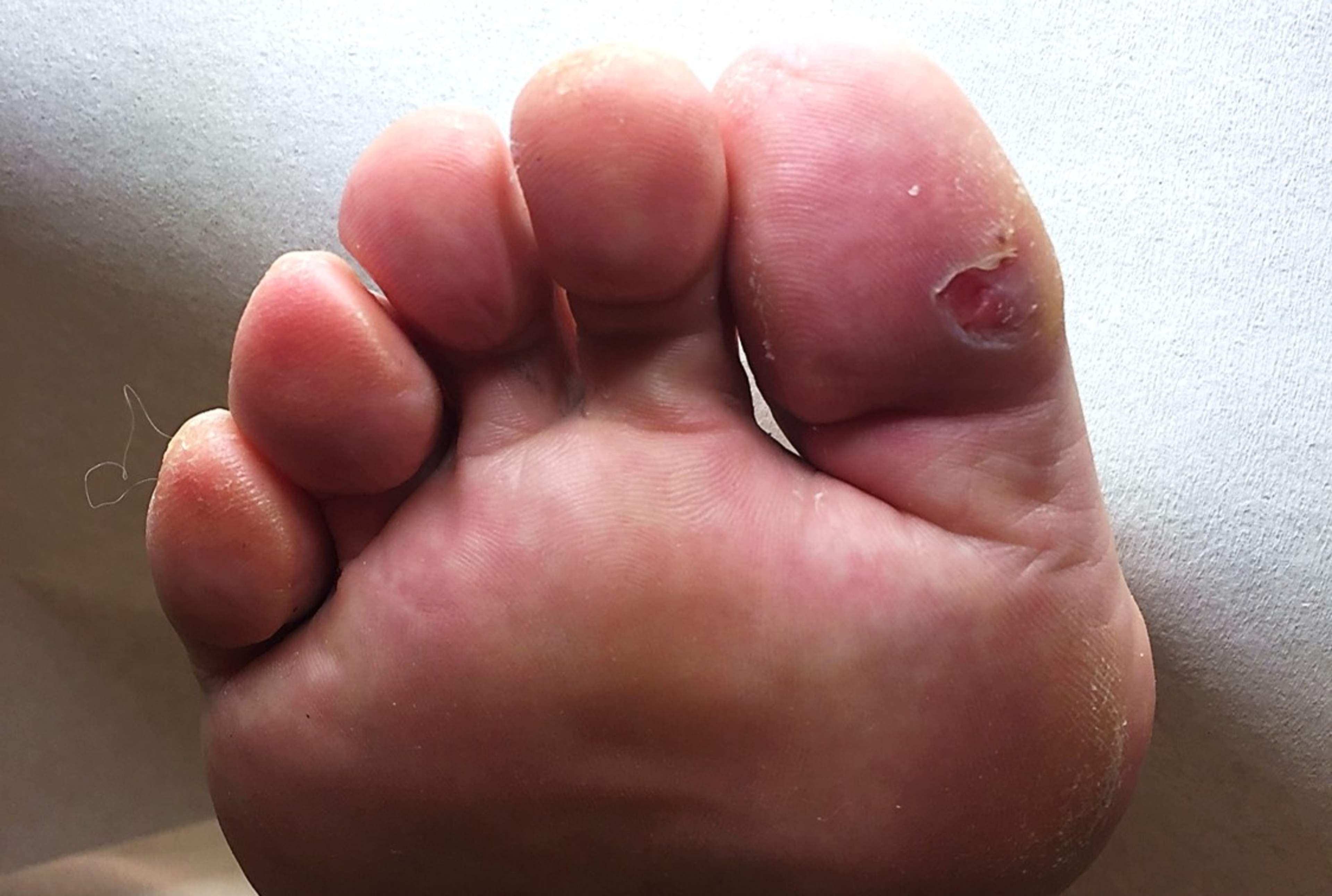
Managing Arterial Ulcers
Diagnosis includes a physical examination, blood pressure measurements at the ankle and arm, and imaging such as ultrasound or CT scans to assess blood flow in the arteries.
Treatment focuses on improving blood supply. This may include stopping smoking, managing diabetes, cholesterol and blood pressure, medications to improve circulation, and referral to a vascular specialist. Some patients may need procedures such as angioplasty or bypass surgery. Compression is usually avoided or used at a lower level to avoid further impairment of arterial blood flow.
Early treatment is important to reduce the risk of deterioration and possible progression to amputation.
Get Specialist Care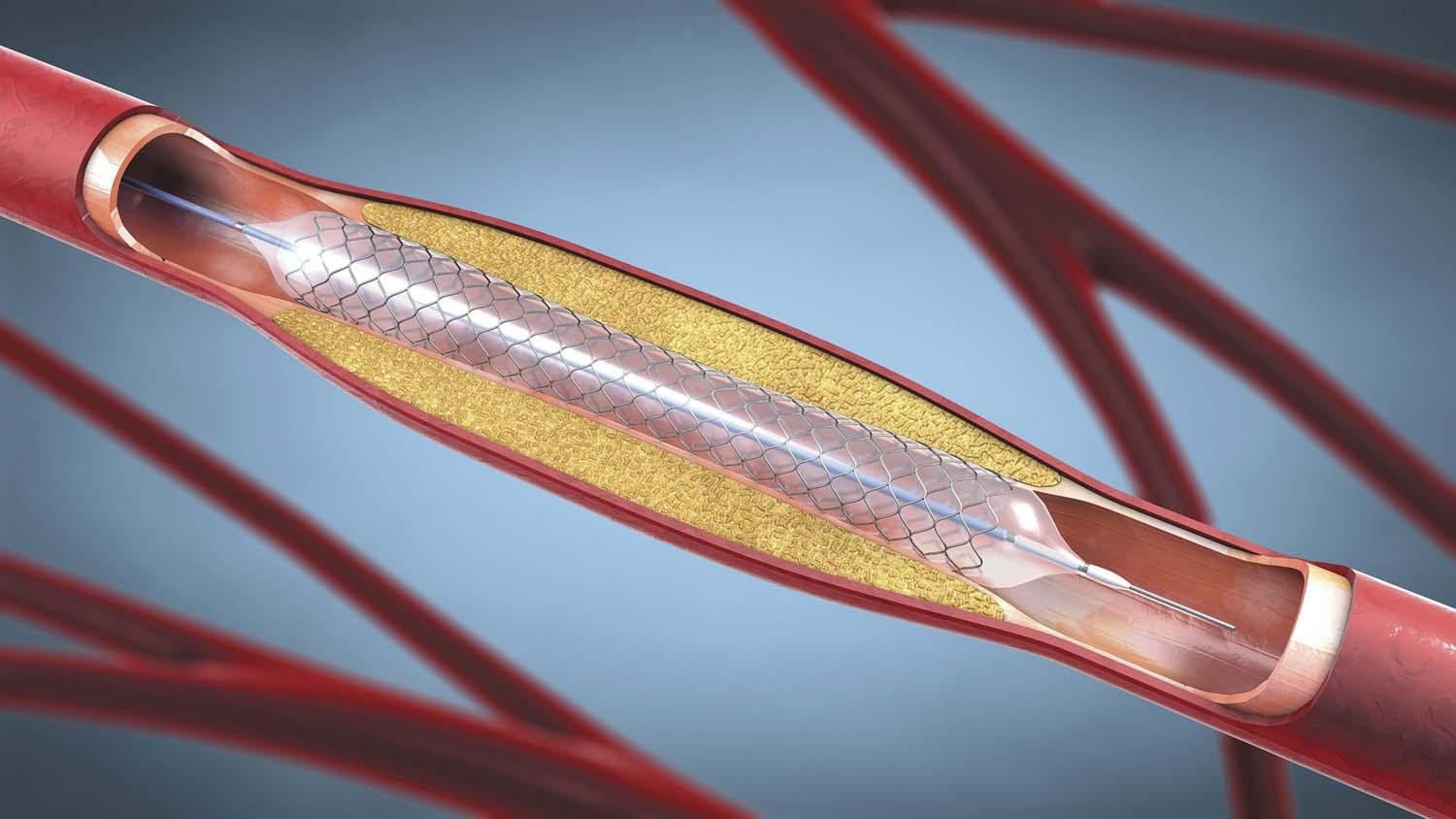
Mixed Arterial and Venous Ulcers
What is a Mixed Ulcer?
A mixed arterial and venous leg ulcer is caused by problems with both the arteries and the veins. This means blood has difficulty reaching the skin and also struggles to return to the heart, making healing slower and more complex.
These ulcers may show features of both types. The leg may be swollen and discoloured, while the ulcer itself may be painful, deeper than a typical venous ulcer, and slow to heal. The surrounding skin may appear shiny or fragile.
An example is an older person with diabetes and varicose veins who develops a painful ankle ulcer that does not respond well to standard compression therapy.
Get a Professional Diagnosis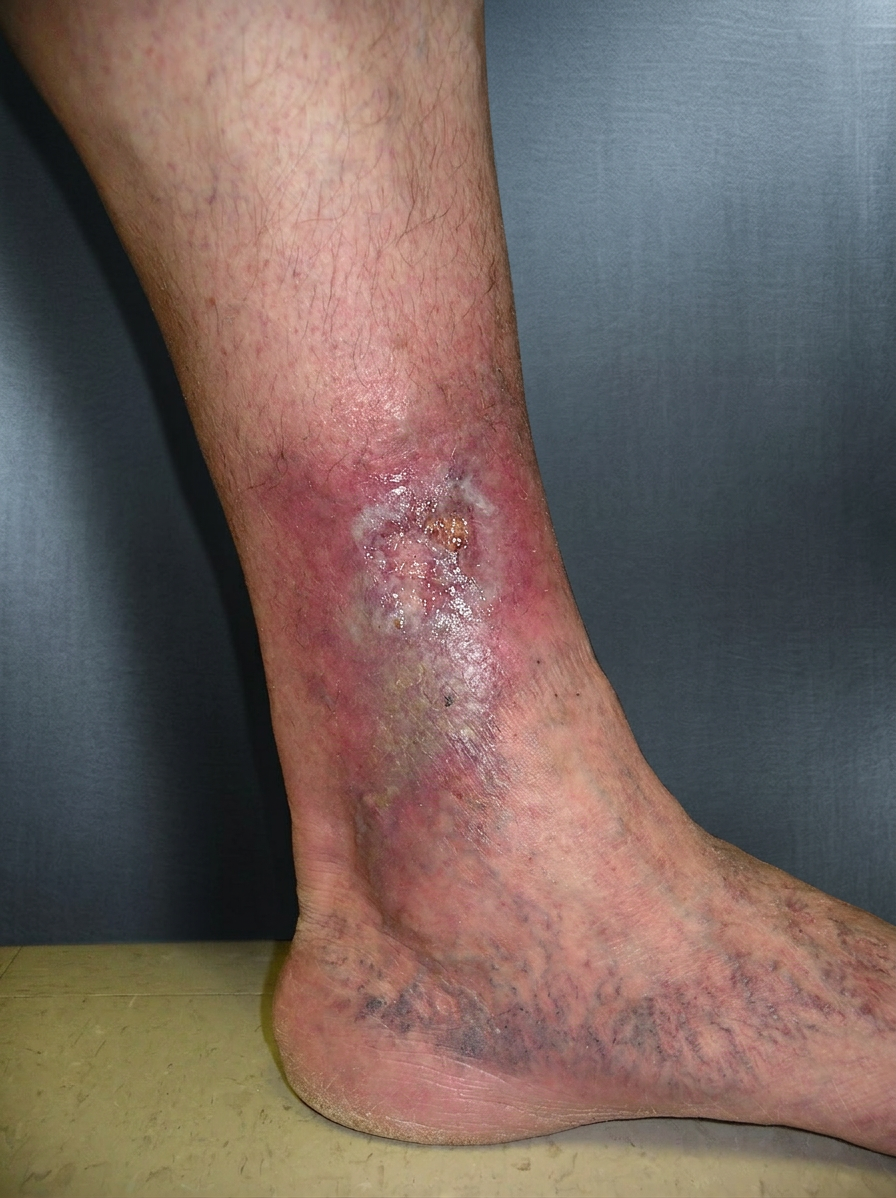
Complex Care Management
Diagnosis usually includes ultrasound scans of both the arteries and veins, as well as ankle blood pressure measurements to assess circulation balance.
Treatment must be carefully tailored and supervised by a vascular surgeon. Low-level compression is often used, but initial treatment will often involve improving arterial blood flow. Once arterial flow has been improved, the level of compression can be increased and any varicose veins can be treated with endovenous ablation (Venaseal, RFA).
These ulcers often take longer to heal and require regular monitoring.
Book an Appointment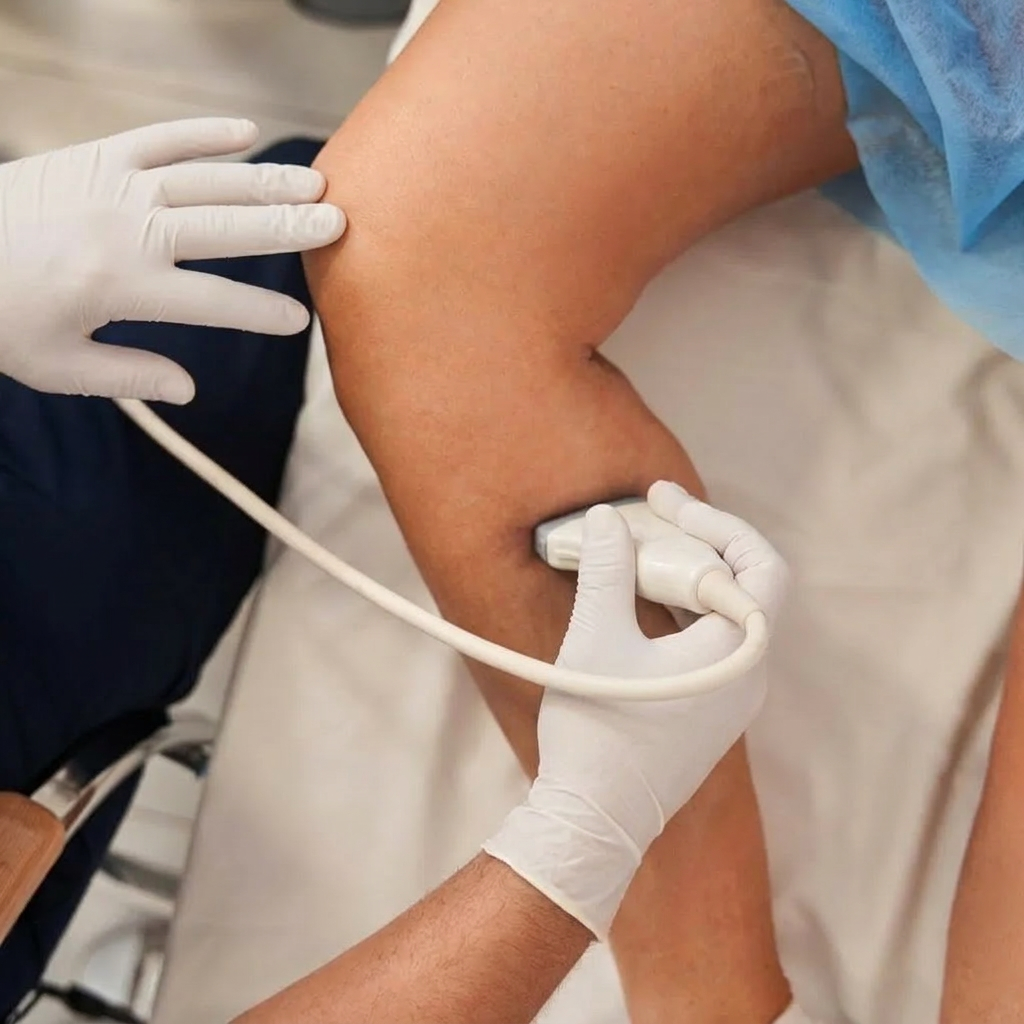
Skin Cancer Ulcers
What is a Skin Cancer Ulcer?
An ulcer caused by skin cancer is an open sore caused by a cancerous change in the skin rather than a circulation problem. Some skin cancers can appear as wounds that do not heal, bleed easily, or slowly grow over time.
These ulcers may look irregular, raised, or have uneven edges or unusual colouring. They may be painless at first but can become sore or tender as they enlarge.
An example is a small scab on the lower leg that repeatedly bleeds and never fully heals, eventually being diagnosed as a type of skin cancer such as squamous cell carcinoma (SCC) or basal cell carcinoma (BCC). Sometimes melanomas can form ulcers.
Book a Skin Check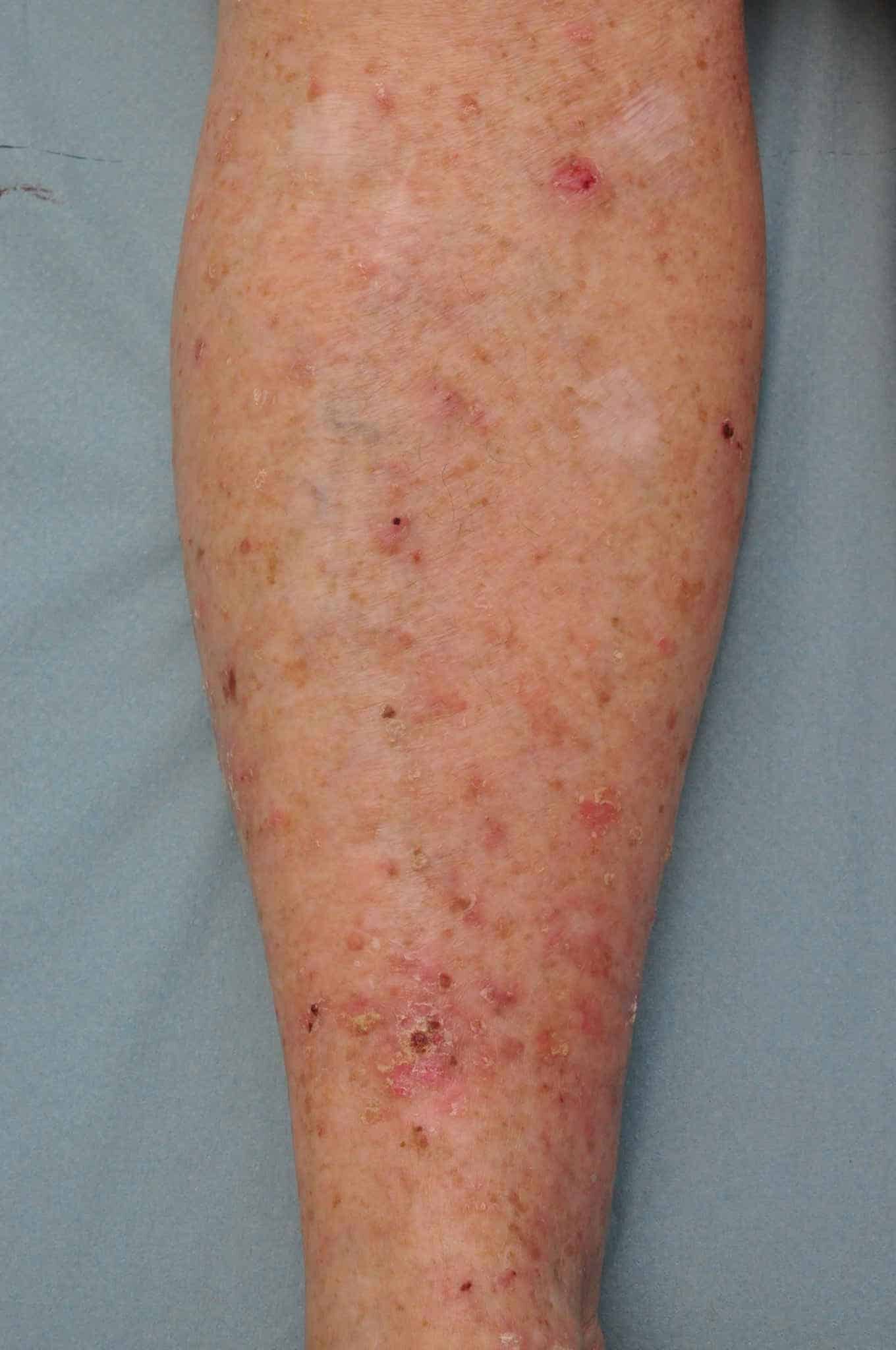
Medical Assessment & Care
Diagnosis requires a medical examination and usually a biopsy, where a small sample of tissue is taken for laboratory testing.
Treatment depends on the type and size of the cancer and may include surgical removal, topical treatments, or referral to a specialist. Early diagnosis and treatment are important for the best outcome.
Any ulcer that does not heal within a few weeks should be assessed by your GP, nurse specialist, or specialist.
Consult a Specialist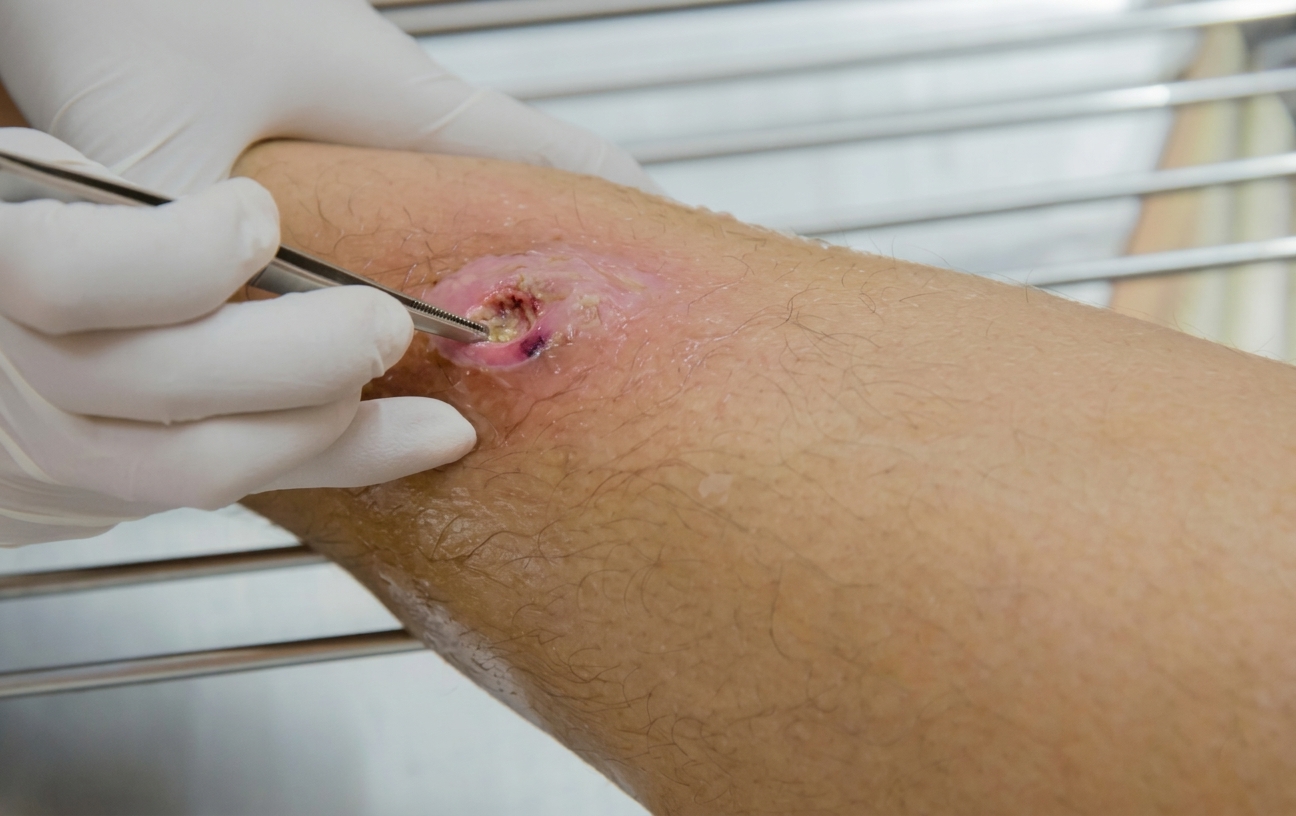
Vasculitis Leg Ulcers
What is a Vasculitis Ulcer?
A vasculitis leg ulcer is caused by inflammation of the blood vessels, which reduces blood flow to the skin and leads to tissue damage and ulcer formation. Vasculitis can be linked to autoimmune conditions (e.g. rheumatoid arthritis, SLE), infections (e.g. hepatitis), reactions to certain medications, blood conditions, and cancers.
These ulcers are often painful and may be associated with other symptoms such as rash, joint pain, fever, fatigue, or general illness. The surrounding skin may appear red, purple, or bruised, and small spots or lumps may also be present nearby.
For example, a person with an autoimmune condition such as rheumatoid arthritis may develop painful skin ulcers along with joint pain and a rash.
Request an Appointment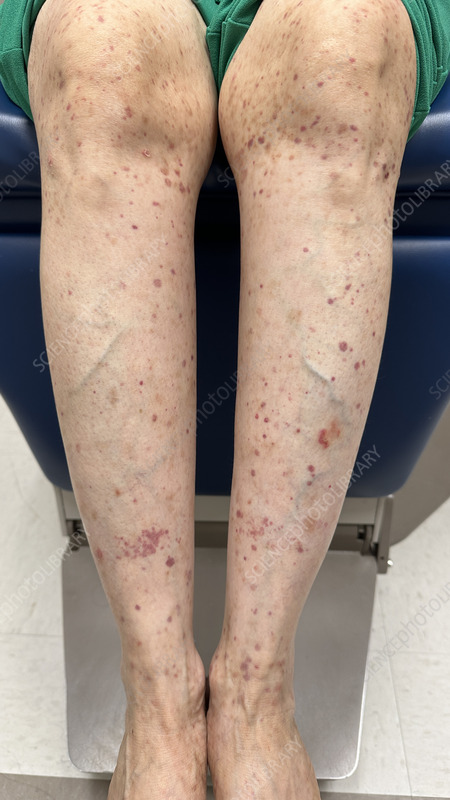
Managing Inflammation
Diagnosis usually involves blood tests, imaging, and sometimes a skin biopsy to confirm blood vessel inflammation and identify the underlying cause.
Treatment focuses on controlling the inflammation with medications such as steroids or other immune-modifying drugs, as well as careful wound care to support healing.
Because vasculitis can be linked to other medical conditions, specialist care and regular monitoring are often required.
Learn More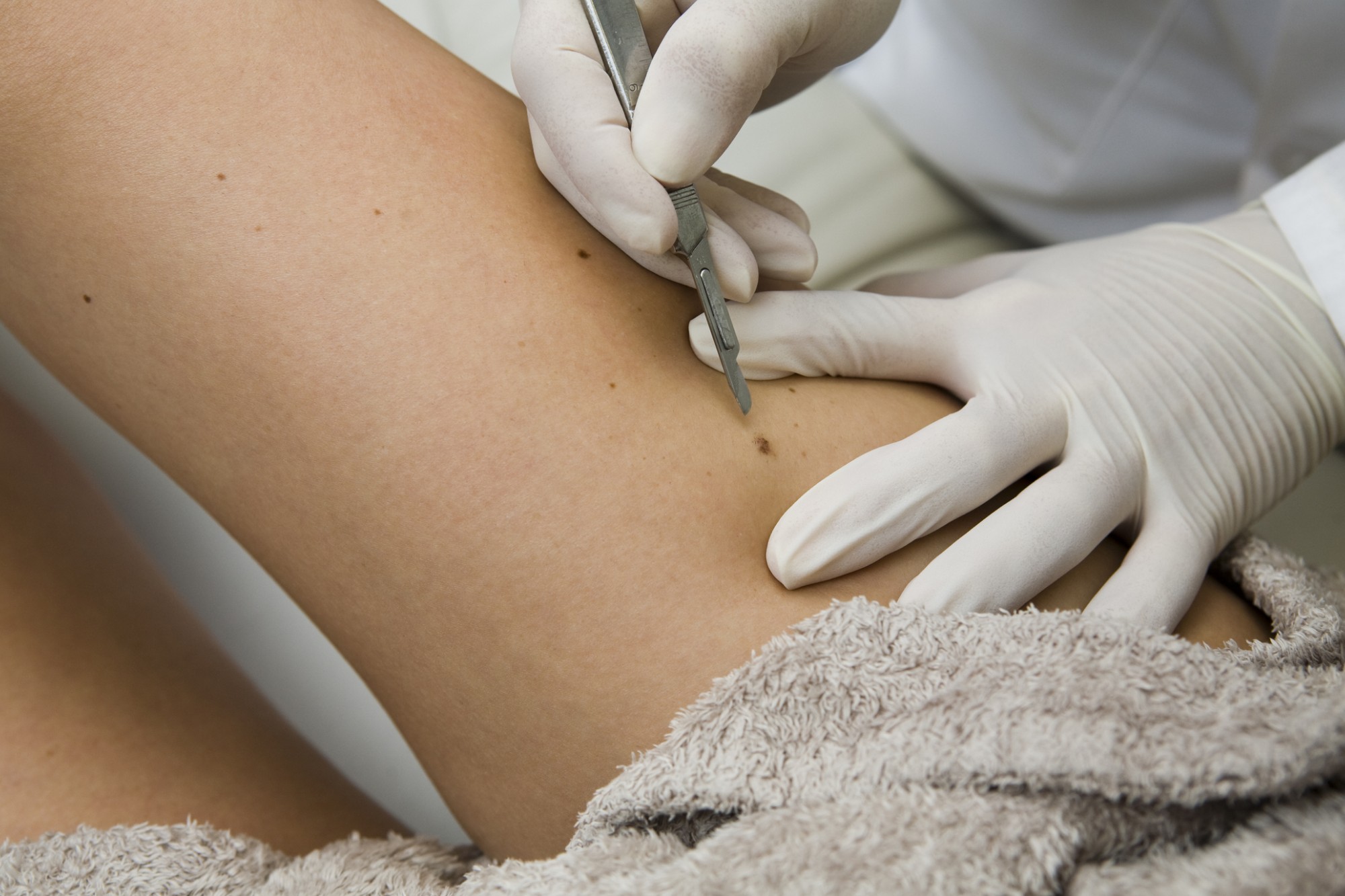
Oedema Leg Ulcers
What is an Oedema Ulcer?
An oedema leg ulcer develops when long-term swelling stretches the skin and reduces its ability to heal. Oedema can be caused by varicose veins and venous insufficiency (leakage), heart failure, kidney disease, lymphatic problems (lymphoedema), or long periods of immobility.
The skin may become tight, shiny, and fragile. Even a small cut or scratch can develop into an open sore. The ulcer is often surrounded by swollen, weeping skin and may be uncomfortable rather than severely painful.
For example, someone with chronic heart failure may develop persistent leg swelling and later notice a small wound on the lower leg that becomes an ulcer.
Assess Your Symptoms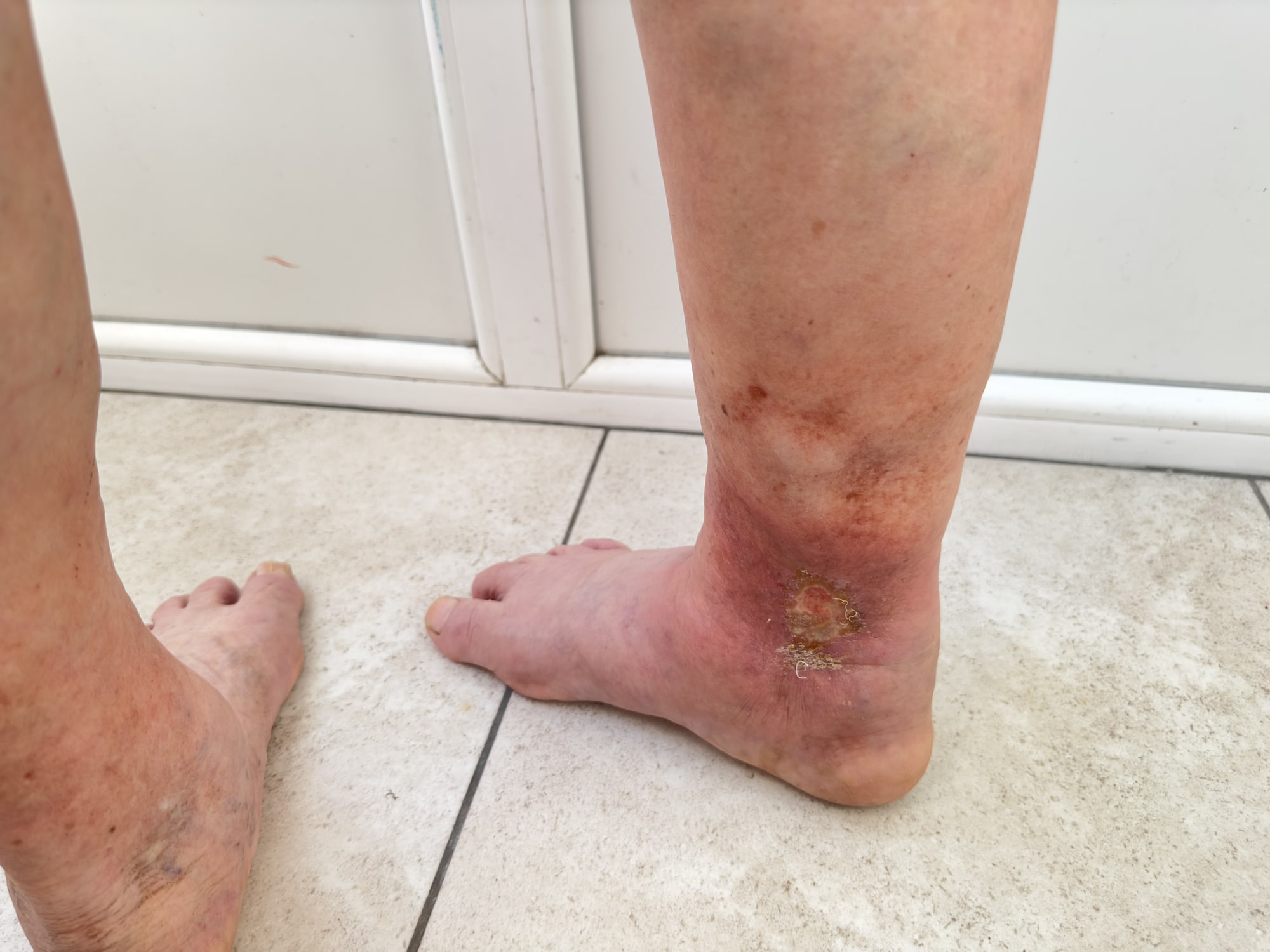
Reducing Swelling & Healing
Diagnosis focuses on identifying the cause of the swelling. This may involve blood tests, heart and kidney assessments, and ultrasound scans.
Treatment includes managing the underlying condition, reducing swelling with elevation and compression bandaging, socks or stockings when appropriate, and careful wound and skin care.
With good control of swelling, healing can improve and future ulcers can often be prevented.
Discover Compression Therapy
Venous Leg Ulcers
What is a Venous Ulcer?
A venous leg ulcer is an open sore on the lower leg or ankle caused by poor blood flow in the veins. Healthy veins use one-way valves to move blood back toward the heart, but when these valves become weak or damaged, blood can pool in the lower legs. This increases pressure inside the veins and leads to fluid and blood cells leaking into the surrounding skin, gradually damaging it and causing an ulcer to form.
Venous leg ulcers most often develop around the inside of the ankle. The surrounding skin may look darkened or brown, feel thick or tight, and may be dry or itchy. The leg is often swollen, especially toward the end of the day. The ulcer itself is usually shallow, irregular in shape, and may leak clear or yellow fluid.
Common examples include people with long-standing varicose veins who develop a small wound after a minor knock, or people who have had a previous blood clot (DVT) and later notice skin changes and an ulcer near the ankle (post-thrombotic syndrome).
Get Expert Help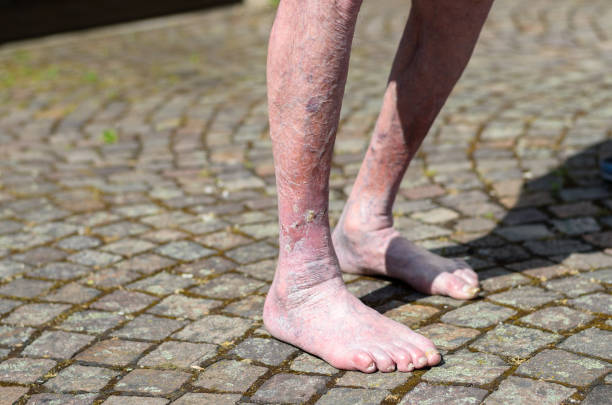
Expert Vein Care
Diagnosis usually involves a physical examination and an ultrasound scan to assess how well the veins and their valves are working. A simple circulation test at the ankle (ankle-brachial index, ABI) is often done to make sure it is safe to use compression therapy.
Treatment focuses on improving blood flow and helping the wound heal. This commonly includes compression bandages or medical stockings, regular wound cleaning and dressings, elevating the leg, and gentle exercise such as walking. Treating underlying vein problems, such as varicose veins with procedures like endovenous ablation (Venaseal, RFA), can significantly improve healing and reduce the risk of recurrence.
With consistent care, many venous leg ulcers heal within a few months. Long-term use of compression stockings and regular follow-up can help prevent the ulcer from returning.
View Vein Solutions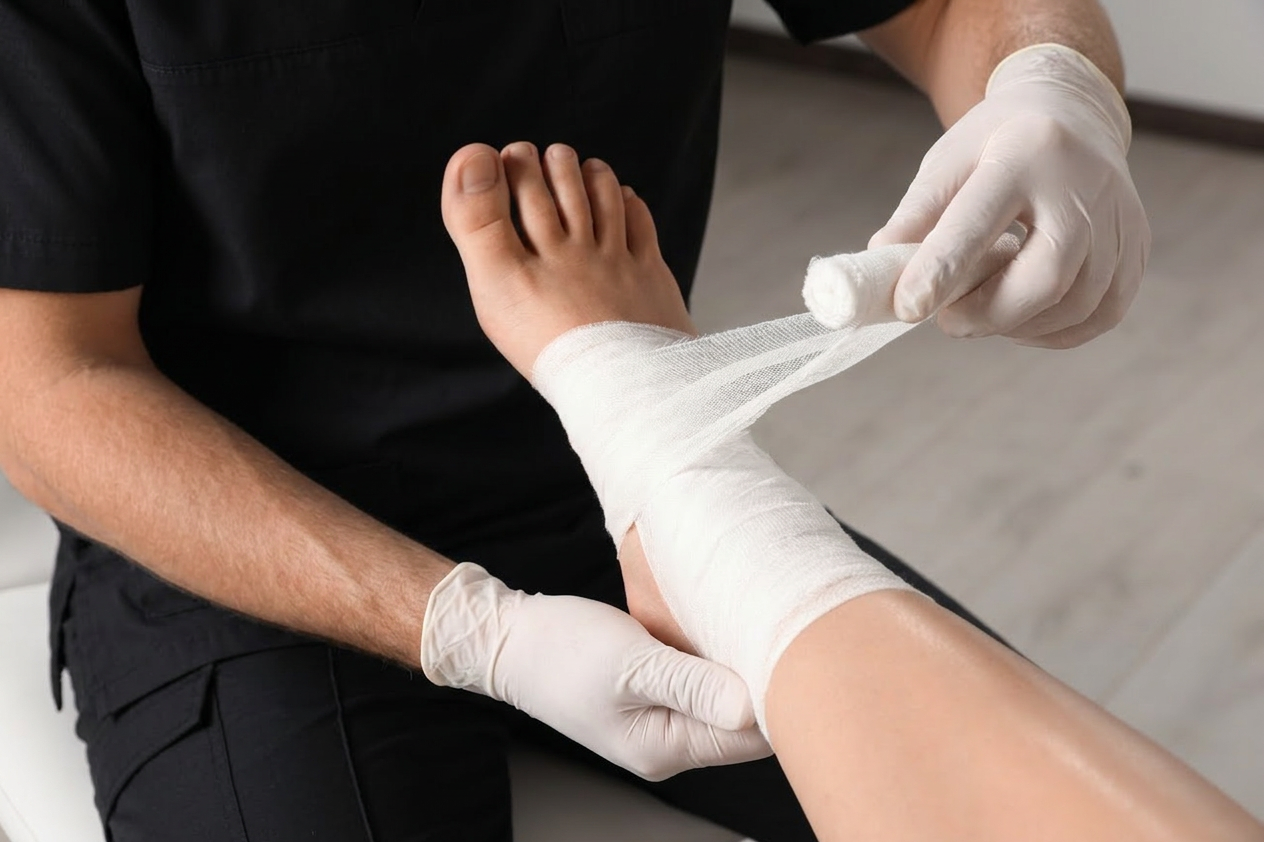
Diabetic Foot Ulcers
What is a Diabetic Foot Ulcer?
A diabetic foot ulcer (DFU) is an open sore or wound that develops on the foot of a person with diabetes. It is usually caused by a combination of poor circulation and nerve damage (neuropathy), which reduces feeling in the feet and makes it easier for small injuries to go unnoticed and worsen over time.
People with diabetes may not feel pain, heat, or pressure in their feet as well as they should. This means a small cut, blister, or area of rubbing from footwear can develop into an ulcer without being noticed. Reduced blood flow can also slow healing and increase the risk of infection.
Diabetic foot ulcers often develop on pressure points such as the ball of the foot, the heel, or the tips of the toes. The surrounding skin may look red, callused, or swollen. The ulcer itself may be shallow or deep and can sometimes expose underlying tissue.
Examples include a blister from a tight shoe that becomes an open wound, or a small cut on a toe that fails to heal and gradually enlarges.
Book a Foot Assessment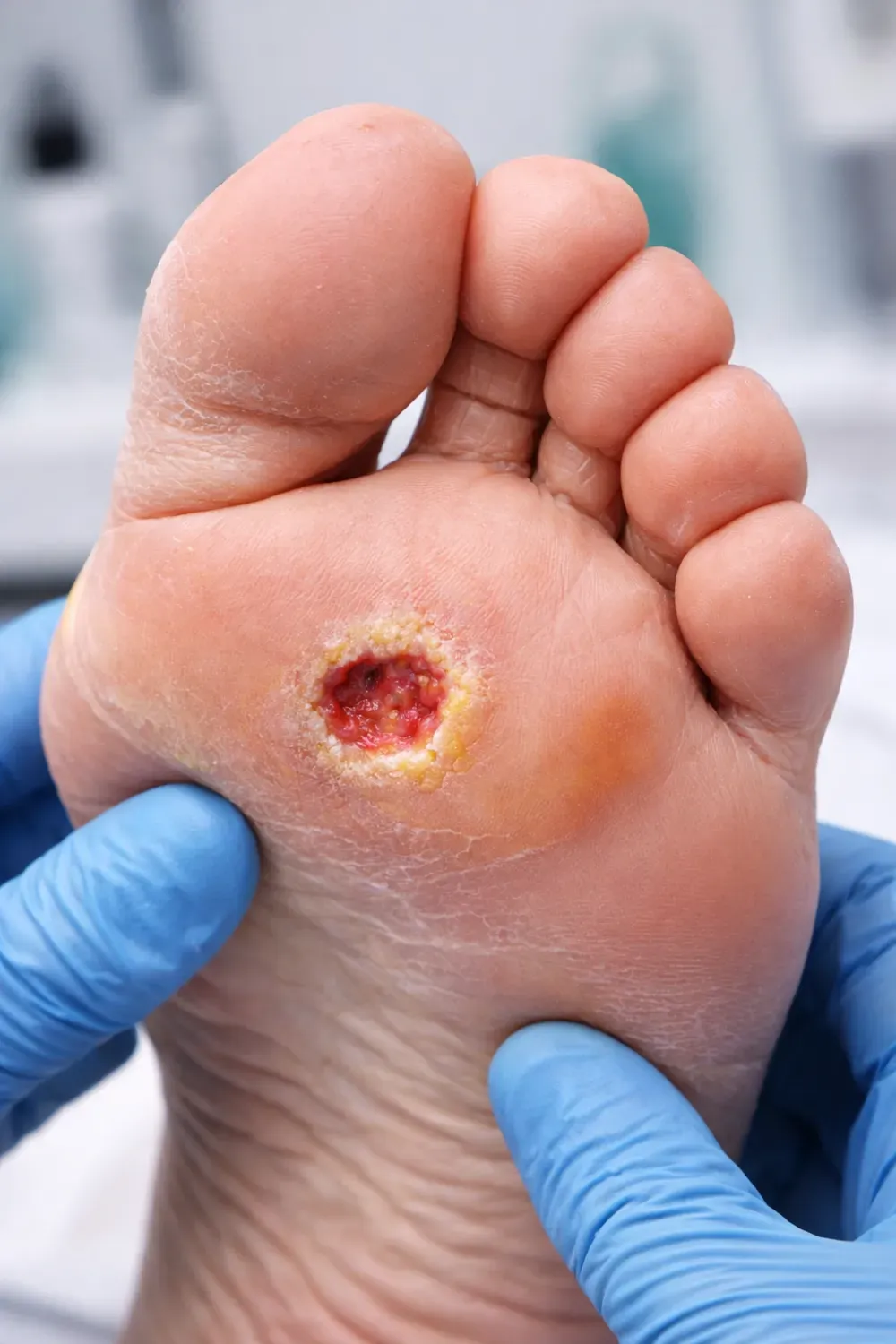
Specialist Diabetic Ulcer Care
Diagnosis usually involves a physical examination of the foot, testing sensation to check for nerve damage, and assessing circulation with blood pressure measurements or ultrasound and CT scans. Management is multidisciplinary, involving teams of vascular surgeons, endocrinologists, podiatrists, ulcer nurse specialists, orthopaedic surgeons, orthotics specialists, and infection disease specialists.
Treatment focuses on protecting the wound and improving healing. This may include regular wound cleaning and dressings, relieving pressure on the area with special footwear or offloading devices, controlling blood sugar levels, and treating any infection with antibiotics. Referral to a multidisciplinary team is often needed.
With early detection and proper care, many diabetic foot ulcers can heal. Daily foot checks, well-fitting footwear, and good diabetes management are important to help prevent ulcers from developing or returning.
Speak to Our Team

Make an Enquiry.
Request a callback or book your initial consultation for ulcer treatment. Referrals are welcome but not always required.
Phone: 0800 45 45 99
Email: info@pulsehealth.nz
Office Address: 1/39 Ghuznee Street, Te Aro 6011, Wellington
